Implants
BREAST RECONSTRUCTION USING IMPLANTS
The implant method for breast reconstruction is a process that typically starts on the day of mastectomy.
GENERAL INFORMATION
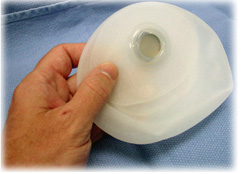
Image: tissue expander. The access port is visible; this is the point that is accessed (through the skin) to fill the expander with saline during the expansion process.
As mentioned previously, the majority of breast reconstructions are now performed as immediate reconstruction. After the oncologic surgeon has completed the mastectomy, the reconstruction process begins with creation of a space behind the pectoralis muscle (chest muscle). This creates a pocket, where the tissue expander will be placed. Several drains are placed within this pocket as well, these come out through the skin under the arm to the side of the breast.
After placement of the tissue expander, most patients go home within 2 days after surgery. While at home, you will be on antibiotics, and will stay on that medicine as long as the drains are still in place. During the 1st or 2nd week after the surgery, the patient is in close contact with Dr. Concannon and his staff, discussing the amount of drainage and deciding when the drains will come out.
After 2 or 3 weeks (usually) we can start the expansion process. The process of tissue expansion to reconstruct the breast mound is very similar to the pregnant abdomen. In clinic, the tissue expander is accessed with a needle, and 60-120cc of saline is placed within the expander. (Saline is a dilute salt water mixture, the same solution that is used for intravenous fluids, and is completely nontoxic and safe for injection).
This is then repeated every week, gradually filling the tissue expander. During these weeks of expansion, the breast mound slowly grows in size; just like the pregnant abdomen, the breast skin stretches and also grows to accommodate the underlying expansion.
Once we have reached the approximate breast mound size that we ultimately want, we will continue to add some more fluid, so that the breast mound is over-expanded in comparison to the final size desired. (Overexpansion makes the ultimate reconstruction easier to perform, and allows a more natural appearing breast after placement of the permanent breast implant).
After we have slightly over-expanded the breast, the woman can “stop being a patient” for approximately four months. During this time, we are allowing the soft tissue to heal prior to proceeding to the next stage (removal of the tissue expander, and placement of the permanent breast implant). At this stage the woman fits into her clothes normally, and does not require bulky and uncomfortable external prostheses.
Choosing the Type of Permanent Implant
![]()
It is time to think about the type of breast implant you want. The main decision point here is whether to choose a silicone gel implant or a saline (salt water filled) implant.
Silicone breast implants have received a tremendous amount of media and legal attention since the early 1990’s. At that time, the FDA turned its attention to the safety of breast implants. Although these silicone gel filled implants had been utilized on hundreds of thousands of women for decades, the FDA was concerned that there was not adequate studies demonstrating that silicone gel implants did not cause harm.
Another piece to this puzzle is the risk/benefit ratio: a greater risk of harm is intuitively allowable, if there is a correspondingly higher potential benefit. One example of this would be the FDA’s approval of a new chemotherapy drug for lung cancer: while the drug itself may carry considerable risk of side effects, it may be acceptable if the potential benefit (saving a life in a lung cancer patient) is great. In the case of breast implants, at least in the FDA at that time, the implication was that there essentially there was no benefit to breast implants, and so therefore any risk is unacceptable.
Since that process started, there has been a great deal of activity from all parties: the implant manufacturers, the surgeons, the researchers, and the plaintiff attorneys. The allegation was made that perhaps there was a higher incidence of auto-immune diseases (such as rheumatoid arthritis, scleroderma, and lupus) in women with breast implants. Breast implants are now the most studied and analyzed surgical implant of any medical device ever created. The end result of years of analysis and study of virtually tens of thousands of woman-years exposure to silicone gel implants has failed to confirm any increased risk for any disease process or problem. It did confirm a reduction in the risk of breast cancer in those women who had breast implants.
I am completely comfortable using silicone gel implants in my patients; I would be comfortable with my own family members having them if they desired. However, my opinion as a surgeon is not important here: what is important is the level of comfort of my patient. If I am asked during this decision process (regarding preference of silicone gel vs. saline filled implants) my preference, the usual response is that “I prefer the silicone gel implant because it makes me look better.” In my opinion, the silicone gel implants have a more natural look and feel, and I think perhaps a better result for that reason. Nevertheless, the patient has to be completely comfortable with her choice: it does not make sense to go through the process of breast reconstruction to have the patient worried about the possible health effects of her implants.
The decision of implant type is completely up to the patient; we can proceed to the second stage of breast reconstruction using either the saline or silicone gel implants.
Currently there are no restrictions on the use of silicone gel breast implants in the United States. For complete information, visit the FDA’s website.
Further options in saline and silicone implants
There are some other choices available to the patient regarding the breast implant. The manufacturers of breast implants supply implants with different surfaces (textured, or smooth) and different shapes. For example, you may select an anatomic shape which is fuller on the bottom, or a round, standard shape. These differences are largely hype, and have little bearing in my experience on the ultimate outcome. My usual choice for implant is smooth round implant (either saline or silicone gel). In my practice, approximately 20% of the women elect to have reconstruction with the saline filled implants, the other 80% select silicone gel.
Tissue expander removal and permanent implant placement
Each successive step in the reconstructive process is simpler and easier on the patient than the preceding step. The second stage procedure is typically done as an outpatient, and the patient may return home after the procedure.
The procedure usually is performed through the previously made incision on the lateral side of the breast. No new scars are made. It is not unusual to make some slight “adjustment” to the reconstructed breast to improve symmetry with the other side; during the expansion phase we may notice that the implant is too high, or low, etc– this can be easily adjusted at the time of the second stage.
The implant method of breast reconstruction is sometimes complicated by capsular contracture. This complication was more commonly seen with older silicone implants and is less common today.
Obtaining symmetry
One of the main goals of the second stage procedure is to obtain symmetry with the contralateral side. If both sides are being reconstructed simultaneously (not too unusual a situation, as often the woman may elect to have a prophylactic mastectomy of the unaffected side at the same time as her mastectomy) this may require a minor adjustment of each side. If the woman’s natural breast remains on the other side, the situation may be that some surgery can be considered for this breast to improve symmetry. For example, the remaining breast may be somewhat ptotic (droopy), and the woman may be more interested in correcting this droopiness rather than trying to recreate that same look with the reconstructed breast. In the past several years, national legislation has mandated that insurance companies cover these procedures for these women in this situation. In general, the possible contralateral surgery may include:
- Breast augmentation (enlargement)
- Breast mastopexy (ptosis correction, droop correction)
- Breast reduction
Each of these procedures can be done during the second stage, and it is preferable to perform them at this time, so that minor adjustments can be done to each side to maximize the opportunity to obtain symmetry. Obviously, it is a good idea to have discussed this plan for other breast surgery with your surgeon far in advance of this operation; I prefer to have this mapped out before the first stage is started, if possible. For example, if the woman desires an augmentation (enlargement) of her native breast, that will need to be taken into account when selecting the size of tissue expander for the reconstructed side, and will impact on the end-point of the expansion process.
After implant placement is completed, I like to allow several months to elapse prior to working on the “finishing touches” of the reconstruction: nipple and areola reconstruction. This is done in 2 minor stages in our clinic procedure room using local anesthesia.
